Nerve Injuries and Myositis Ossificans associated with Supracondylar Humerus Fracture
Vol 1 | Issue 1 | July-Sep 2015 | page:30-32 | Maulin Shah, Maulik Patel.
Authors : Maulin Shah[1], Maulik Patel[2].
[1] Consultant Pediatric Orthopedic Surgeon, Orthokids Clinic, Ahmedabad, India.
[2] Clinical Fellow , Orthokids Clinic, Ahmedabad, India.
Address of Correspondence
Dr. Maulin Shah
OrthoKids Clinic,
Kamdhenu House, Opp. Apang Manav Mandal,
Drive-in Road, Memnagar, Ahmedabad – 380 052.
Email : orthokidsclinic@gmail.com
Abstract
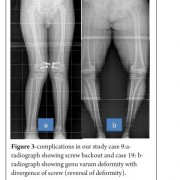
Background: Angular deformities around the knee joint in skeletally immature children are treated with methods of reversible hemiepiphysiodesis like staples, transphyseal screw and eight plate. Hemiepiphysiodesis using Eight plate has showed good results with advantage being faster correction, less complications and can be used in younger age.
Methods: The aim of this retrospective study is show the efficacy of eight plate application and its complication rate. Nineteen patients (37 physes) (unilateral: 3; bilateral: 16) with angular deformity were treated with eightplate application. Seven with pathological physes and twelve with idiopathic physes. Outcome assessment was done clinically with calculation of intermalleolar /intercondylar distance and radiologicaaly with mechanical and anatomical axis. Correction achieved was considered when anatomical/mechanical axis were within normal limits and intermalleolar/intercondylar distance was less than 5 cm.
Results: The average age of intervention was 7.4±2.96 years (range 2.4 -11.2years). Rate of correction of IMD/ICD was 1.14 cm per month. Rate of correction of mechanical axis was 0.76 o per month. Rate of correction of anatomical axis was 1.04o per month. The average duration of eight plate removal 12.4 months (range 7-24 months).There were two complications one patient with screw backout and other with overcorrection.
Conclusion: Reversible hemiepiphysiodesis using eight plate is and effective method with minimal complications and faster rates of correction. Idiopathic physes show faster rates of correction than pathological physes. Physeal growth arrest is not seen with eight plate application. Larger data and long term follow up is required to assess the rebound deformity after eight plate removal.
Keywords: Reversible, hemiepiphysiodesis, angular deformity, eight plate.
Introduction
Supracondylar humerus fractures are the most common upper limb injury amongst children. Due to the vicinity of the important nerves in this area, nerve injuries are frequently encountered with these fractures.
Incidence
Incidence of nerve injuries associated with supracondylar humerus fractures is reported to be 10 to 20% in different published studies. Most of these injuries can be identified preoperatively by proper clinical evaluation. Anterior interosseous nerve is the most commonly encountered nerve injury in extension type of fractures with incidence of 12 to 15%.[1-3] Radial nerve injury is second most common in this group with occurrence about 8%. Ulnar nerve injury is least commonly seen in extension injuries & approximate incidence is about 3%[4,5]. Flexion type of supracondylar fractures have more common association with Ulnar nerve injury.
Fracture morphology & Nerve Injuries
In extension type of fractures, median nerve is injured with postero-lateral displacement & radial nerve is injured with postero-medial displacement of fracture. In a study of 59 consecutive cases of type -III fractures, Crowford and collegues reported that 87% of median nerve injuries were associated with postero-lateral displacement and all radial nerve injuries were associated with postero-medial displacement[6]. The rate of acute neurologic injury in ipsilateral supracondylar humerus and forearm fractures is almost twice than that found in patients with isolated supracondylar humerus fractures. In a series of 150 patients with ipsilateral injuries, Muchow et. al. observed that the overall incidence of nerve palsy was 18.9% when a forearm fracture required reduction compared with only 7.3% in a forearm fracture that was not reduced[7]. In a series of 26 open supracondylar humerus fractures, Ozkul et. al. reported the incidence of nerve injury to be as high as 34%. A careful pre-operative evaluation to identify the nerve injury is thus advocated in open injuries[8]. Correlation was also found between severity of fracture type and incidence of nerve injury. Gartland type- II had 7%, type -III had 19% and type-IV had 36% chances of nerve injuries[9]. Nerve interposition between fracture fragments can cause failure of closed reduction. In a series of 41 failed closed reduction, Fleuriau-Chateau et. al. reported that 15 patients had entrapment of Median Nerve or Radial Nerve. Thus, incidence of nerve injury in failed closed reduction is approximately 35%[10].
Clinical Evaluation for Nerve Injury
Although it is difficult to do complete neurological evaluation in an injured child, it is very important to note the status of pre-operative movements. Trainees should note the ability of a child to carry out specific tasks rather than pointing specific nerve injuries. Median nerve injury can be identified by loss of thumb & index finger inter-phalangeal flexion. “Pointing index finger” while the child is asked to flex the fingers is a cardinal sign. Loss of extension at Metacarpo-phalangeal joints of fingers & thumb extension is suggestive of Radial Nerve involvement. Clawing of ulnar fingers & loss of adduction-abduction of fingers suggests Ulnar Nerve injury. Sensory deficits are difficult to indentify in acute injuries[11].
Types of Nerve Injuries
Most of the nerve injuries associated with supracondylar fractures are neuropraxic in nature. It is produced by the perineural fibrosis induced by direct compression of the fractured bony fragment. These injuries have good potential of spontaneous recovery. Complete transaction of the nerve is rare and radial nerve is the most commonly involved in this category[12]. Nerve can get entrapped in callus and produce symptoms of nerve injury. Radiologically, it gives appearance of a hole in the bone & is known as “Metev’s Sign”[3]. Compartment syndrome is an uncommon but known complication of Supracondylar fracture in today’s era. Increased pressure in the compartment causes nerve ischemia. Median Nerve paresis is the most commonly observed in this category. Majority of Ulnar Nerve injuries are caused Iatrogenically rather than direct injury.
Iatrogenic Nerve Injuries
Ulnar nerve injury is observed more as iatrogenic injury rather than post traumatic injury. Recent literature reports iatrogenic Ulnar nerve injury incidence to be 3% – 4%[13]. Cross pinning configuration has shown more chance to contracting Ulnar nerve injury compared to lateral pinning.[14] Passage of Ulnar nerve between Olecranon and the medial epicondyle makes it more prone to injure when medial pin I s passed in the cubital groove. Skaggs et. al. reported that hyperflexion of elbow increases chance of Ulnar nerve injury threefold & they recommend reducing elbow flexion after placing the first lateral pin in extension variety of supracondylar fractures[9]. Majority of instances the Ulnar nerve is injured by direct trauma or compression of sheath due to winding while drilling of wire. Shtarker et. al. used Ulnar nerve monitoring through electrical stimulation during & at the end of medial pinning. They found this technique safe, simple & easily applicable. In a series of 138 patients, by using this method, they did not notice any Ulnar nerve injury after doing crossed pinning[15]. Mulpuri et. al. found a mini-open technique useful to reduce the incidence of iatrogenic Ulnar nerve injuries while doing cross pinning. They recommended retraction of Ulnar nerve under direct vision by a 1.5 cm medial incision before introducing medial pin[16]. Literature reports that about 17-30% children have Ulnar nerve instability. An ultrasound study of the Ulnar nerve anatomy done by Eraze & colleagues, suggested that the incidence of anterior subluxation & dislocation of the Ulnar nerve is significantly high in patients with generalized hyperlaxity compared to normal population. They suggested that the ultrasound evaluation and assessment of ligamentous laxity are additional tools which can identify children at risk of iatrogenic nerve injury[17]. Iatrogenic radial nerve injury is rare and associated with piercing by medial pin as it exists through the anterolateral cortex. Most of these injuries are neuropraxia and spontaneous recovery occurs usually. Medial pin penetration in the opposite cortex should be limited to 1 mm to 2mm to prevent radial nerve injury[18].
Treatment approach to Nerve Injuries
Most nerve injuries are neuropraxias in nature & they generally show spontaneous recovery in 3 months time. Franklin et. al. suggested need of immediate exploration in nerve palsy with accompanying pulselessness[12]. Reducible fractures with nerve injuries should be treated with closed reduction and close follow up. Irreducible fractures with nerve deficits require open reduction to rule out nerve entrapment. If nerve deficit is found within a few hours of cross pinning then pin should be removed and nerve should be explored. It is advisable to change to lateral pinning. Nerve deficit after a few weeks of cross pinning can be managed by pin removal and observation for 5 to 6 months. If recovery does not occur then neurolysis is the mainstay of treatment. Rarely nerve grafting is indicated.
Conclusion
Nerve injuries associated with supracondylar humerus fracture is a frequent occurrence. One should have high degree of suspicion about it & a careful pre-operative clinical examination is needed to report it. Median nerve injury is the most common nerve injury associated with extension variety of fractures. Incidence significantly increases in open fractures, ipsilateral forearm fractures & fractures with vascular compromise. Ulnar nerve injury is commonly happen as iatrogenic injury due to cross pinning. A mini-open technique or ultrasound evaluation or electric nerve monitoring during surgery are recommended tools to reduced its incidence. Most of the nerve injuries are neuropraxias and they spontaneously resolve by 6 months. Small percentage of patients may need nerve exploration & repair.
Myositis ossificans in Supracondylar humerus fractures
Wilkins reported 1.4% incidence of myositis ossificans in his meta-analysis of 470 cases of supracondylar humerus fractures[19]. Brachialis is the commonest muscle to get involved and causes restriction of range of motion[20]. High energy trauma, manipulation by bone setter, aggressive postoperative physiotherapy and overzealous dissection while open reduction are the risk factors[21]. In early stage, patients present with pain, redness, local warmth and swelling. In late stage, once the ossification settles, bony mass is palpable separately from the underlying bone and it causes restriction of motion at the elbow[22]. On plain radiographs, myositis looks like calcification in its early stages. Mature myositis mass demonstrates well defined outer shell of the bone, commonly at anterolateral aspect of the elbow. CT scan is helpful to confirm[23]. Early stage is treated by analgesics & anti-inflammatory medicines and restriction of passive exercises. Mature myositis mass should be excised completely. Material should be sent for the histopathological examination[22,24]. Preoperative or early postoperative radiotherapy has been reported to prevent myositis ossificans occurrence in at-risk patients. Prophylactic dose should be between 600 and 1000 cGy[25, 26].
References
1. Cramer KE, Green NE, Devito DP. Incidence of anterior interosseous nerve palsy in supracondylar humerus fractures in children. Journal of Pediatric Orthopaedics. 1993;13(4):502-505.
2. Spinner M, Schreiber SN. Anterior interosseous-nerve paralysis as a complication of supracondylar fractures of the humerus in children. Journal of Bone Joint Surgery (Am). 1969; 51(8):1584-1590.
3. McGraw JJ, Akbarnia BA, Hanel DP, et al. Neurological complications resulting from supracondylar fractures of the humerus in children. Journal of Pediatric Orthopaedics.1986; 6(6):647-650.
4. Skaggs DL, Hale JM, Bassett J, et al. Operative treatment of supracondylar fractures of the humerus in children. The consequences of pin placement. Journal of Bone Joint Surgery (Am). 2001; 83A(5):735-740.
5. Cheng JC, Lam TP, Shen WY. Closed reduction and percutaneous pinning for type III displaced supracondylar fractures of the humerus in children. Journal of Orthopaedic Trauma. 1995; 9(6):511-515.
6. Crowford CC, Peters WM, John EB, James KR, Michael MB. Neurovascular injury and Displacement in Type III Supracondylar Humerus Fractures. Journal of Pediatric Orhtopaedics. 1995 Jan:Feb ;15(1) : 47-52
7. Muchow RD, Riccio AI, Garg S, Ho CA, Wimberly RL. Neurological and vascular injury associated with supracondylar humerus fractures and ipsilateral forearm fractures in children. Journal of Pediatric Orthopaedics. 2015 March;35(2):121-5.
8.Ozkul E , Gem M, Arslan H, Alendar C, Demirtas A, Kisin B. Surgical treatment outcome for open supracondylar humerus fractures in children. Acta Orthopaedics Belgium. 2013 October;79(5):509-513.
9. Joiner ER, Skaggs DL, Arkader A, Andras LM, Lightdale-Miric NR, Pace JL, Ryan DD. Iatrogenic nerve injuries in the treatment of supracondylar humerus fractures: are we really just missing nerve injuries on preoperative examination? Journal of Pediatric Orthopaedics. 2014 June; 34(4):388-92.
10. Fleuriau-Chateau P, McIntyre W, Letts M. An analysis of open reduction of irreducible supracondylar fractures of the humerus in children. Canadian Journal of Surgery. 1998; 41(2):112-128.
11. RW Culp, AL Osterman, RS Davidson, T Skirven, FW Bora. Nerural injuries associated with supracondylar fractures of humerus in children. Journal of Bone Joint Surgery.1990 Sep; 72(8):1211-1215.
12. Franklin CC, Skaggs DL. Approach to the pediatric supracondylar humeral fracture with neurovascular compromise. Instructional Course Lectures. 2013;62:429-33.
13. Cheng JC, Ng BK, Ying SY, Lam PK. A 10-year study of the changes in the pat- tern and treatment of 6,493 fractures. Journal of Pediatric Orthopaedics. 1999;19:344-50.
14. Wilkins KE. Fractures and dislocations of the elbow region. In: Rockwood CA Jr, Wilkins KE, King RE, editors. Fractures in children. Volume 3. 3rd edition. New York: JB Lippincott; 1991. p 526-617.
15. Shtarker H, Elboim-Gabyzon, Bathish E, Laufer Y, Rahamimov N, Volpin G. Ulnar nerve monitoring during percutaneous pinning of supracondylar fractures in children. Journal of Pediatric Orhtopaedics. 2014March;34(2):161-5.
16. Mulpuri K, Tritt BL. Low incidence of ulnar nerve injury with crossed pin placement for pediatric supracondylar humerus fractures using a mini-open technique. Journal of Orthopaedic Trauma. 2006 March;20(3);234
17. Erez O, Khalil JG, Legakis JE, Tweedie J, Kaminski E, Reynolds RA. Ultrasound evaluation of ulnar nerve anatomy in the pediatric population. Journal of Pediatric Orthopaedics. 2012 September ;32(6):641-6.
18. Sairyo Koichi, Henmi Tatsuhiko, Kanematsu Yoshiji, Nakano Shunji, Kajikawa Tomomasa. Radial Nerve Palsy Associated with Slightly Angulated Pediatric Supracondylar Humerus Fracture. Journal of Orthopaedic Trauma. 1997 April;11(3):227-229.
19. Wilkins KE. Fractures and dislocations of the elbow region. In: Rockwood CA, Wilkins KE, King RE. Fractures in Children. 3rd edition. New York: JB: Lippincott; 1991; 509-28.
20. Naranje S1, Kancherla R, Kannan A, Malhotra R, Sharma L, Sankineani SR. Extraarticular bony ankylosis in a child with supracondylar fracture of humerus. Chinese Journal Traumatology. 2012;15(5):300-2.
21. Hartigan BJ1, Benson LS. Myositis ossificans after a supracondylar fracture of the humerus in a child. American Journal of Orthopedics. 2001 Feb;30(2):152-4.
22. Spinner, Robert J.; Jacobson, Scott R.; Nunley, James A. Case Report Fracture of a Supracondylar Humeral Myositis Ossificans. Journal of Orthopaedic Trauma: June 1995; 183-277
23. Zeanah WR, Hudson TM. Myositis ossificans: radiologic evaluation of two cases with diagnostic computed tomograms. Clinical Orthopedic Related Research. 1982 Aug;(168):187-91.
24. Augustus Thorndike Jr. Myositis ossificans traumatica. Jounal of Bone Joint Surg Am, 1940 Apr; 22 (2): 315 -323.
25. Brady LW. Radiation-induced sarcomas of bone. Skeletal Radiology 1979;4:72-8.
26. Kim JH, Chu FC, Melamed HQ, Huvos A, Cantin J. Radiationinduced soft-tissue and bone sarcoma. Radiology 1978;129:501-8.
| How to Cite this Article: Shah M, Patel M. Nerve Injuries and Myositis Ossificans associated with Supracondylar Humerus Fracture. International Journal of Paediatric Orthopaedics July-Sep 2015;1(1):30-32. |