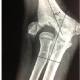
Novel Method of Treating Elevated Compartment Pressures Post Intraosseous Cannulation of Tibia
Volume 2 | Issue 2 | May-Aug 2016 | Page 38-40|Eamon O Ceallaigh, Francis O’Neill, Jim Kennedy, Jacques Noel
Authors :Eamon O Ceallaigh [1], Francis O’Neill [2], Jim Kennedy [2], Jacques Noel [2]
[ 1] Mater Misericordiae University Hospital,Dublin Ireland
[2] Our Lady’s Children’s Hospital Crumlin, Dublin Ireland
Address of Correspondence
Dr Eamon O’Ceallaigh
Our Lady’s Children’s Hospital Crumlin, Dublin Ireland
Email: eamonoceallaigh@rcsi.ie
Abstract
Introduction: Vascular access is a vital task in the resuscitation of a critically ill child. Although peripheral intravenous access is the traditional method for gaining vascular access, this can be challenging in patients with circulatory collapse.
Today IOI (Intra Osseous Infusion) is accepted as standard equipment on paediatric and adult rescue carts. IOI is recommended in Advanced Cardiac Life Support and Pediatric Advanced Life Support treatment protocols as alternative means of vascular access in the event that IV cannulation is delayed or not feasible. The conventionally recommended site for IOI is the proximal tibia.
Case Report: We report the case of a 6 month old boy with meningococcal septicaemia who was admitted to ICU for resuscitation that had an attempted intraosseous cannulation in his left leg with intravenous fluids administered in the ambulance en route. On arrival at the hospital, it was noted that the left foot was swollen and tense and an alternative site for administration of fluids was obtained. An orthopaedic review was sought for possible compartment syndrome left foot. Stryker needle measurements of intracompartmental pressures within the foot were elevated. The decision was then made to apply an eschmark bandage to the left foot and lower leg and to elevate the leg for 2-3 minutes with this in place. After removing the eschmark bandage, the intracompartmental pressures were remeasured and found to have returned to acceptable levels.
Conclusion: We believe that if compartment syndrome is being considered because of the clinical examination and/or elevated intracompartmental pressures in patients post IOI, it may be worth employing this technique with the eschmark bandage before proceeding to surgical decompression as this technique is far less invasive than surgical decompression and if successful, as in this case, can lower intracompartmental pressures quite significantly and quickly.
Keyword: Paediatrics, Orthopaedics, Resuscitation, Musculosketelal
Introduction
Vascular access is a vital task in the resuscitation of a critically ill child.[1,2] Although peripheral intravenous access is the traditional method for gaining vascular access, this can be challenging in patients with circulatory collapse and it has been demonstrated that experienced emergency department personnel can require more than 10 minutes to gain IV access in such cases[3].
Tocantins and O’Neill established in 1941 that the bone marrow cavity of a long bone was a possible site of vascular access and in the 1940s[4] and early 1950s, Intra Osseous Infusions (IOI) were used extensively in children who required repeated blood transfusions and antibiotic therapy[5] IOI has also been shown by radionucleotide technique to deliver fluids as rapidly as intravenous techniques [6] However intraosseous infusion fell out of popularity in the 1950s due to the advent of plastic IV catheters.[5]
Today IOI is accepted as standard equipment on paediatric and adult rescue carts. IOI is recommended in Advanced Cardiac Life Support and Pediatric Advanced Life Support treatment protocols as alternative means of vascular access in the event that IV cannulation is delayed or not feasible.[2,7]
Studies have demonstrated that the use of IOI can decrease the time needed to obtain vascular access in paediatric patients in cardiac arrest.[8,9] and that the rate of vascular access in paediatric cardiac arrest patients is higher for IOI (83%) than for all other forms of IV access.[10]
However, there are potential complications associated with IO infusion and these include osteomyelitis, cellulitis, fracture at IO-line site, compartment syndrome, and fat embolism. [14,15,16,17]
It is the complication of compartment syndrome that we would like to discuss further in this case report.
Case Report
We report the case of a 6 month old boy with meningococcal septicaemia who was admitted to ICU for resuscitation. While in the ambulance on route to the hospital, paramedics had attempted an intraosseous cannulation in the child’s left leg. Uncertainty exists as to whether the cannula was correctly sited but intravenous fluids were administered through this cannula. On arrival at the emergency department, it was noted that the left foot was swollen and tense and an alternative site for administration of fluids was obtained. After resuscitation and admittance to ICU, the orthopaedic team were asked to review the patient with regard to a swollen discoloured left foot. The child was fully intubated and otherwise stable at this stage. On examination, the left foot was swollen and tense to palpation. There was good capillary refill in all the toes and a dorsalis pedis pulse was palpable. It was impossible to assess discomfort or pain in the foot at this stage as the child was fully intubated. As a full clinical examination was not possible due to the clinical condition of the child, it was decided to use a stryker needle to measure intracompartmental pressures within the foot with the intention of determining if there was a case for compartment syndrome in the foot. It is now accepted that there are 9 compartments within the foot[12] The stryker was initially placed perpendicular to the skin at the medial aspect of the foot, at the base of the first metatarsal and only advanced 1cm approx to measure the medial compartment. Once that measurement was taken, the needle was subsequently advanced deeper to measure the pressure within the central compartment. One measurement was taken laterally from the lateral compartment. Due to the small size of the foot and relatively large size of the needle, it was decided against individually measuring the other remaining compartments as there would be multiple large puncture wounds in a relatively small foot. A collective measurement was taken from the dorsal aspect of the foot and we are aware that this may not accurately represent the instrinsic compartments. Initial measurements with the stryker needle revealed that the intracompartmental pressure on the dorsal aspect of the foot was 15mmHg while the pressure on the plantar aspect of the foot (medial, central, lateral) was 37mmHg and this result was confirmed by 2 different individuals independently measuring compartment pressures within the foot. Diastolic blood pressure at the time of measurement of the compartment pressures was 56mmHg.
Compartment Syndrome can be considered when the pressure difference between diastolic blood pressure and intracompartmental pressure is less than 30mmHg or also when absolute interstitial pressure is greater than 30mmHg.
The decision was then made to apply an eschmark bandage to the left foot and lower leg and to elevate the leg for 2-3 minutes with this applied. The reason for attempting this course of action was that we had reasoned that the raised intracomparmental pressure was the direct result of the fluid that had leaked into the soft tissues within the compartment after the administration of fluid through the incorrectly sited IOI cannula and that by applying the eschmark bandage, we may be able to force some of this fluid out of the compartment and back into the vascular system.
Once the eschmark bandage was removed, the intracompartmental pressures within the foot were again measured with the stryker needle. These results revealed an improvement in pressures with the dorsal compartment reading 12mmHg and the pressure recorded on the plantar aspect of the foot (medial, central and lateral compartments) reducing to 21mmHg. The diastolic blood pressure was 58mmHg while these repeat measurements were being taken. This measurements was taken twice to help ensure that they was accurate. Clinically, the foot also looked better and was less tense to palpation. The foot was subsequently elevated and monitored. The foot continued to improve clinically and surgical decompression for compartment syndrome was not necessary.
Discussion
Intra Osseous Infusion is a proven method of delivering urgently needed fluids to a patient and this method of delivery works because the rich vasculature of long bones transports the fluids and medications to the central circulation. Sinusoids within the marrow of long bones function as rigid conduits that do not collapse in the presence of hypovolemia. Blood passes into the venous channels of the medulla and then leaves the bone through nutrient or emissary veins entering the general circulation.
The conventionally recommended site for IOI is the proximal tibia[2] The tibial tuberosity should be located by palpation just below the patella and the recommended insertion site is the relatively flat area approximately 2cm distally and slightly medial to the tibial tuberosity. Although this site is usually distal to the growth plate, it is still recommended that the needle be angled 10–15 degrees caudally to avoid injury to the growth plate. The patient’s leg should be restrained and a small sandbag placed under the knee. The area should be cleaned and draped using sterile technique. Proper IO placement in the marrow canal can be confirmed by three methods. First, the needle should stand on its own without support. Second, after unscrewing the inner trocar from the needle, bone marrow should be able to be aspirated through the needle. Third, a 5–10-mL saline bolus injection should enter with little resistance and without evidence of extravasation; this can be confirmed by carefully observing the calf area for acute swelling or discoloration. Only one IO attempt should be made in each bone. Multiple punctures in the periosteum may result in extravasation of fluid into the soft tissues. However, if the needle becomes plugged with soft tissue, it may be removed, and a new needle may be inserted through the same cannulation site.[11]
It is recommended that IO needles should not be placed at fractured extremities because extravasation will occur at fracture sites. The tibia and distal femur are recommended sites in infants and children younger than 6 years. These sites are easily identified by topical landmarks, and the bones are superficially located. Needles inserted in these locations traverse tissue planes devoid of important structures, and the marrow cavity is relatively large. These sites are also physically removed from other resuscitative efforts, such as airway management and chest compressions. Also it is worth noting that secure vascular access should be obtained before the functioning IO needle is removed.
As this case report demonstrates, compartment syndrome can become a complication of IO insertion and this has been previously reported [14,15,17]. We speculate that this resulted primarily from extravasation of fluid into the muscular compartments. The potential causes for this extravasation include incomplete penetration of the cortex, penetration of the needle through the posterior aspect of the cortex, extravasation through a previous IO puncture site, and extravasation through the foramina of the nutrient vessel [17]
Precautionary measures that reduce the incidence of compartment syndrome and allow for its early recognition include correct placement of the IO line to reduce the amount of fluid extravasation. A fresh, large-bore needle should be used to facilitate bone penetration, prevent blockage of the lumen, and withstand bending forces. Multiple breaches of the cortex should be avoided, and the needle should be passed only through the near cortex. Aspiration of marrow contents confirms accurate placement, and free flow of fluid into the osseous cavity should be noted. Plain radiographs can also be used to confirm placement. If improper placement is confirmed, and the cortex has been breached, the site should be well dressed, and insertion can be attempted at another site. It is important that the affected limb be immobilized during use of the IO line to prevent dislodgement of a properly placed needle. The cannula should be secured to the extremity with a noncircumferential dressing to prevent. If possible, the circumference of the extremity at the level of the IO site should be measured serially. Although not immediately life-threatening, IO-line complications can be associated with extensive morbidity. If there is any concern that compartment syndrome is developing, the IO line should be removed immediately, and the appropriate surgical or orthopaedic service should be consulted.
We believe that if compartment syndrome is being considered because of the clinical examination and/or elevated intracompartmental pressures in patients post IOI, it may be worth employing this technique before proceeding to surgical decompression. If successful, as in this case, can lower intracompartmental pressures quite significantly and quickly. Whilst we do not anticipate any major complications unique to this technique, if it is unsuccessful and surgical decompression is delayed the patient may develop the complications of late compartment syndrome. As such, we would advise very close clinical monitoring post-bandage application and low threshold for surgical decompression if the compartment pressures do not lower quickly. If the compartment syndrome is not due to extravasation post IO insertion, we would not expect this technique to work and surgical decompression would most likely be needed.. As such, we are not suggesting this novel technique is a panacea for compartment syndrome but should only be considered in a patient who has developed compartment syndrome post IO insertion and does not have another likely cause for compartment syndrome.
Unfortunately, given the emergent nature of our case, we are unable to provide photographic evidence of our novel treatment as patient care and treatment was the priority at the time and the idea of case report was formulated afterwards. We would like to confirm however that we stand over the authenticity of the case.
We would like to report this technique with the eschmark bandage for lowering intracompartmental pressures in cases of extravasation of fluid into the soft tissue in the case of IOI before proceeding with surgical decompression. This technique is far less invasive than surgical decompression and if the pressure can be lowered significantly, as in this case, the need for proceeding to surgical decompression can be negated.
References
1. Hazinski MF, Cummins RO, Field JM (eds).Basic life support for health care providers. In: Handbook of Emergency Cardiovascular Care for Healthcare Providers. Dallas TX: American Heart Association, 2002, pp 1-2, 96.
2. American College of Surgeons (eds). ATLS, Advanced Trauma Life Support for Doctors, Student Manual. Chicago IL: American College of Surgeons, 1997, pp 12, 97.
3. Rosetti V, Thompson BM, Aprahamian C, Darin JC, Mateer JR. Difficulty and delay in intravascular access in pediatric arrests [abstract]. Ann Emerg Med. 1984;13:406.
4.Tocantins L, O’Neill J. Infusions of blood and other fluids into the general circulation via the bone marrow. Surg Gynecol Obstet. 1941;73:281-7.
5. Rosetti VA, Thompson BM, Miller J, Mateer JR, Aprahamian C. Intraosseous infusion: an alternative route of pediatric intravascular access. Ann Emerg Med. 1985;14:885-8.
6. Cameron JL, Fontanarosa PB, Passalaqua AM. A comparative study of peripheral to central circulation delivery times between intraosseous and intravenous injection using radionucleotide technique in normovolemic and hypovolemic canines. J Emerg Med. 1989;7:12
7. Chameides L, Hazinski MF (eds). Intraosseous Cannulation. In: Textbook of Pediatric Advanced Life Support. Dallas TX: American Association of Pediatrics–American Heart Association,
1994, pp 5-6.
8. Glaeser PW, Losek JD, Nelson DB, et al. Pediatric intraosseous infusions: impact on vascular access time. Am J Emerg Med. 1988;6:330-2.
9. Kanter RK, Zimmerman JJ, Strauss RH, Stoeckel KA. Pediatric emergency intravenous access: evaluation of a protocol. Am J Dis Child. 1986;140:132-4.
10. Brunette DD, Fischer R. Intravenous access in pediatric cardiac arrest. Am J Emerg Med. 1988;6:577-9.
11. Neal CJ, McKinley DF. Intraosseous infusion in pediatric patients. J Am Osteopath Assoc. 1994;94(1):63-6.
12. Manoli A 2nd, Weber TG. Fasciotomy of the foot: an anatomical study with special reference to release of the calcaneal compartment. Foot Ankle 1990;10:267-75.
13. Launay F, Paut O, Katchburian M, Bourelle S, Jouve JL, Bollini G. Leg amputation after intraosseous infusion in a 7-month-old infant: a case report. J Trauma. 2003;55(4):788-790.
14. Vidal R, Kissoon N, Gayle M. Compartment syndrome following intraosseous infusion. Pediatrics. 1993;91(6):1201-1202.
15. Burke T, Kehl DK. Intraosseous infusion in infants. Case report of a complication. J Bone Joint Surg Am. 1993;75(3):428-429.
16. Günal I, Köse N, Gürer D. Compartment syndrome after intraosseous infusion: an experimental study in dogs. J Pediatr Surg. 1996;31(11):1491-
1493.
17. Galpin RD, Kronick JB, Willis RB, Frewen TC. Bilateral lower extremity compartment syndromes secondary to intraosseous fluid resuscitation.
J Pediatr Orthop. 1991;11(6):773-776.
| How to Cite this Article: Ceallaigh EO, O’Neill F, Kennedy J, Noel J. Novel Method Of Treating Elevated Compartment Pressures Post Intraosseous Cannulation of Tibia. International Journal of Paediatric Orthopaedics May-Aug 2016;2(2):38-40. |
(Abstract) (Full Text HTML) (Download PDF)